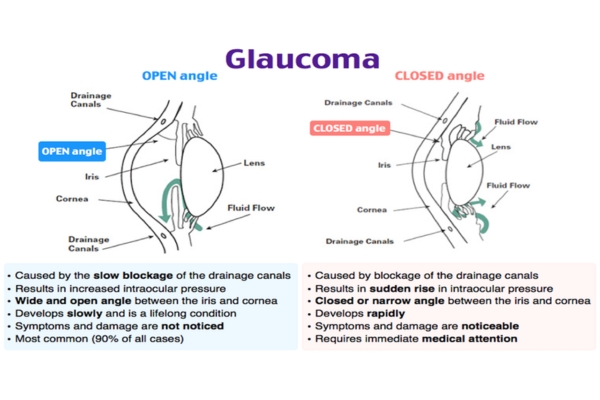
Aqueous humor flows between the iris and the lens,and through pupil,enter the Anterior Chamber. The angle formed by Cornea and Iris is known as “Angle of Anterior Chamber,” which has different structures, one of them is Trabecular meshwork. Trabecular meshwork is a very tiny sponge-like tissue, only one-fiftieth of an inch wide, though which Aqueous humor gets drained into the system. When this drain becomes clogged, aqueous cannot leave the eye as fast as it is produced, causing the fluid to back up. But since the eye is a closed compartment, this `sink´ doesn´t overflow; instead, the backed-up fluid causes increased pressure to build up within the eye. We call this open (wide) angle glaucoma.
To understand how this increased pressure affects the eye, think of your eye as a balloon. When too much air is blown into the balloon, the pressure builds, causing it to pop. But the eye is too strong to pop. Instead, it gives at the weakest point, which is the site in the sclera at which the optic nerve leaves the eye.
The optic nerve is one of the cranial nerves and part of the central nervous system and carries visual information from the eye to the brain. It is made up of over one million nerve axons, which are nerve fiber extensions of the retinal ganglion cells. When the eye pressure is increased and/or other inciting factors exist, the optic nerve becomes damaged and the retinal ganglion cells undergo a slow process of cell death termed “apoptosis.” The death of the retinal cells and degeneration of the nerve fibers results in permanent vision loss. That is why early diagnosis and treatment of glaucoma can help prevent blindness.
The aqueous humor also provides the necessary pressure to help maintain the shape of the eye. We call this intraocular pressure or IOP. As you will read, maintaining the right amount of pressure within the eye is very important to protecting your vision. Measuring the IOP is one of the ways your eye doctor tests for glaucoma.
Who is at Risk:
- Family History –As Glaucoma is a Genetic Disease, family history is very important. If someone is diagnosed with Glaucoma, all family members who are blood related should undergo regular detailed eye examination after 35 years of age
- Race- African, Hispanic, Latino and Asian decent
- High Refractive error like High Myopia
- History of Diabetes
- History of very high or very low blood pressure
- Regular/Long term use of certain medicines like Steroid/Cortisone etc.
- A previous eye injury
- Thin central Cornea
- Age above 40 years
Types of Glaucoma:
- Open Angle Glaucoma- it can be Primary or Secondary Glaucoma.
Here the angle of AC is open along with damage to optic nerve and field of vision.
Patient generally do not realize until field of vision reduces remarkably and that is why it is a silent killer disease, as it is generally irreversible.
Open Angle Glaucoma is initially managed by medicaltreatment. Despite all medical management, if Glaucoma still progresses or if there is poor compliance for whatever reason, then Laser &/or surgical management is advised.
- Closed Angle Glaucoma- it can be Acute and Chronic, Primary and Secondary Glaucoma.
Acute Angle Closure Glaucoma- patient comes to emergency with sever redness, pain with sudden loss of vision. It is treated with Laser Iridectomy/Surgical Iridectomy.
With regular detailed eye examination, it can be diagnosed that patient is prone to develop Acute attack of Angle closure Glaucoma- and in this cases Prophylactic Laser Iridectomy is performed to avoid this attack.
Angle Closure Glaucoma, in primary stage, is managed by Iridectomy treatment (Laser/surgical Iridectomy). In chronic cases medical management &/or surgical treatment is recommended.
- Secondary Glaucoma-
All secondary Glaucoma whether Open or Angle Closure Glaucoma, the cause is determined with detailed Eye Examination along with detailed systemic evaluation.
Along with Glaucoma management, the cause of Glaucoma also needs attention and treatment to prevent further damage.
Comprehensive Eye Checkup for Glaucoma Diagnosis:
To rule out Glaucoma, following tests are very important.
- Intraocular Pressure (IOP)- IOP measurement is done by Non-contact Tonometer and then confirmed by Goldman’s Applanation Tonometry (GAT) whenever needed
- Thickness of the central cornea (CCT)- CCT is measured by Pachymetry
- Gonioscopy: The angle in the eye where the iris meets the cornea (Angle of Anterior Chamber)- Angle of AC is examined by Gonioscopy. By placing the Gonio lens AC angle is examined whether it is open or closed and any other abnormalities
- Shape, Size and Color of the Optic Nerve- To evaluate optic nerve, generally dilated Retina Examination done by Ophthalmoscopy
- The complete field of vision- Field of vision is examined by Perimetry-Visual Field Test. Since the primary symptom of glaucoma, is a progressive decrease in peripheral vision, one of the most important tests is a visual field. In the simplest terms, a visual field detects how dim of a light can be seen in the patient’s peripheral vision
- Complete nerve fiber layer imaging- is done by OCT (Optical Coherence Tomography) of Optic nerve and Macula.
Management of Glaucoma:
- The goal of any treatment is to prevent loss of vision, as vision loss from glaucoma is irreversible. The good news is that glaucoma can be managed if detected early, with medical, Laser and/or surgical treatment. If detected in time, then most people with glaucoma will not lose their sight.
- As mentioned in different types of Glaucoma, there are different ways Glaucoma can be managedand are recommended depending on the type of glaucoma, stage of glaucoma and extent of damage. Like Eye Drops, Tablet, Surgical Procedures, Laser procedures, Micro or Macro Glaucoma Implants- either single or in combination.
- Regular eye checkup, as recommended by your Glaucoma Specialist, is very crucial.
- Control of DM, Hypertension, Hypotension, Sleep Apneaetc.
What Can I Do to Decrease My Chances of Going Blind?
- Glaucomatous blindness is preventable with the currently available treatments.
- Using the medications as prescribed, and regular hospital visits are crucial to prevent damage by Glaucoma progression.
- It is best to monitor the pressure three to four times per year, repeat visual fields at least annually and take photographs of the optic nerve every one to two years.
- Some of these office visits will be brief pressure checks whereas others may include your annual eye exam, visual fields, photos of your optic nerves or imaging of your optic nerve with a scanning laser ophthalmoscope or electrodiagnostic studies.
- You can also help protect the vision of family members and friends who may be at high risk for glaucoma – especially, African Americans over age 40 and everyone over age 60.
- Encourage all blood related family members to have an eye examination through dilated pupils every year, especially after 35 years of age, as Glaucoma is a genetic disease.
- Routine detailed eye examination after 40 years of age is very important to check overall health of our eye.